Snoring Veterans Disability Benefits: Complete Guide to VA Claims and Sleep Apnea Treatment
Quick Answer
Veterans with service-connected sleep apnea can receive VA disability benefits ranging from 0% to 100%, depending on severity and treatment requirements. Currently, only about 25% of veteran sleep apnea claims are approved on first submission, but the condition affects one in five veterans compared to just 5% of civilians. Successful claims require documented medical evidence linking the condition to military service, including exposure to burn pits, deployment stress, or service-related injuries.
Last updated: May 18, 2026
Key Takeaways
- Veterans are four times more likely to develop sleep apnea than civilians, with rates jumping from 5% to 20%
- VA disability ratings for sleep apnea range from 0% (documented but asymptomatic) to 100% (requires tracheostomy)
- The most common rating is 50%, awarded when you require a CPAP or similar breathing assistance device
- Between 2008 and 2010, veteran sleep apnea claims increased by 61%, and the trend continues upward
- Burn pit exposure, combat stress, and deployment conditions are recognized service-connection factors
- Three out of four initial claims are denied, making proper documentation and sometimes legal help essential
- Treatment options range from lifestyle changes and anti-snoring mouthpieces to CPAP machines and surgery
- Over 90% of veterans with post-deployment issues experience sleep disturbances
If you’re a veteran struggling with snoring, daytime exhaustion, or witnessed breathing pauses during sleep, you’re not alone—and you deserve both medical treatment and the disability benefits you’ve earned.
This guide walks you through understanding sleep apnea, navigating the VA claims process, and finding effective treatment solutions.

What Is Sleep Apnea and Why Does It Matter for Veterans?
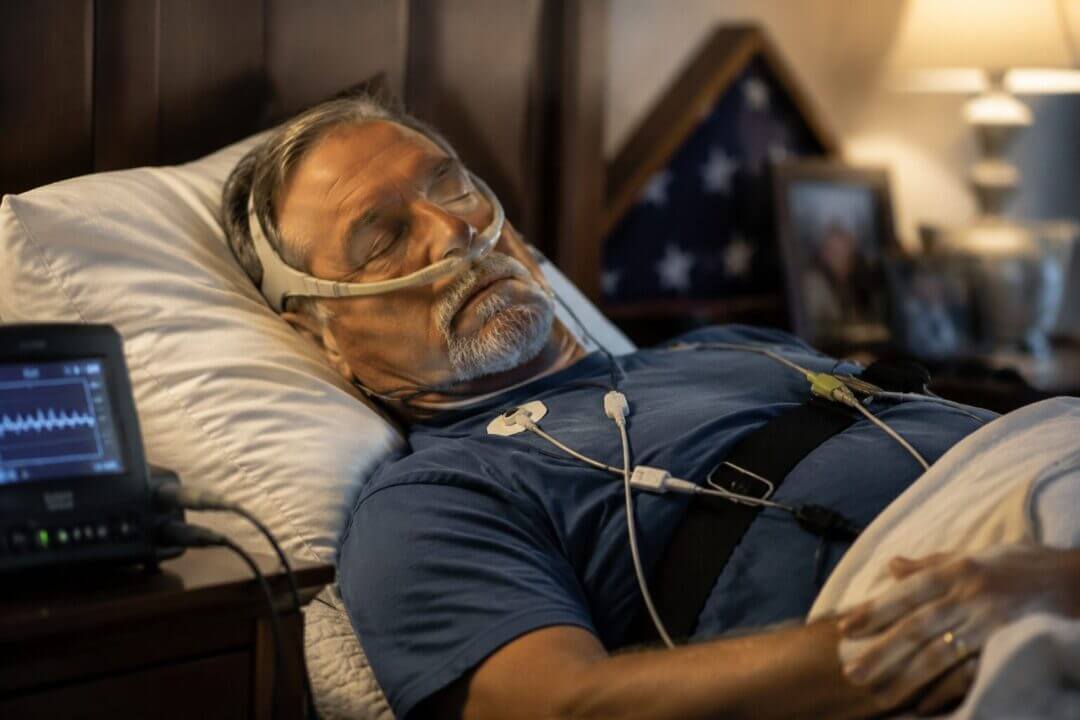
Sleep apnea is a chronic condition where your breathing repeatedly stops or becomes dangerously shallow during sleep. These pauses last anywhere from a few seconds to over a minute and can occur 5 to 100+ times per hour in severe cases.
When breathing stops, your brain jolts you from deep, restorative REM sleep into lighter sleep stages. You might not fully wake up, but your body does—repeatedly, all night long. The result is fragmented sleep that leaves you exhausted, irritable, and at higher risk for serious health problems.
Two main types exist:
- Obstructive Sleep Apnea (OSA): Your airway physically collapses or becomes blocked during sleep. This is the most common type, accounting for roughly 84% of cases. The loud snoring and gasping sounds come from air forcing past the obstruction.
- Central Sleep Apnea (CSA): Your brain fails to send proper breathing signals to your muscles. Less common, usually quieter, and often linked to other medical conditions or medications.
Many veterans have mixed sleep apnea—a combination of both types.
Why veterans face higher risk:
Military service creates multiple risk factors that civilians rarely encounter. Deployment exposes you to burn pits, dust storms, and airborne particulates that damage airways. Combat stress and PTSD disrupt normal sleep architecture. Irregular sleep schedules during deployment train your body into poor sleep patterns. Physical injuries, especially to the head, neck, or jaw, can alter airway structure.
The numbers tell the story: one in five veterans develops sleep apnea versus one in twenty civilians. That’s a 400% increase in risk.
How Sleep Apnea Affects Your Daily Life and Health
Untreated sleep apnea doesn’t just make you tired—it systematically damages your body and mind.
Immediate daily impacts include:
- Severe daytime drowsiness that makes driving dangerous (you’re 2.5 times more likely to have a car accident)
- Difficulty concentrating or remembering things
- Morning headaches from oxygen deprivation
- Irritability and mood swings
- Decreased job performance
- Relationship strain from loud snoring
Long-term health consequences:
Your body needs oxygen. When breathing stops repeatedly, your blood oxygen drops and your heart works harder. Over months and years, this leads to:
- High blood pressure (present in 50% of sleep apnea patients)
- Increased stroke risk (2-3 times higher)
- Heart disease and irregular heartbeat
- Type 2 diabetes (sleep apnea makes insulin resistance worse)
- Weight gain (poor sleep disrupts hunger hormones)
- Depression and anxiety
- Cognitive decline
For veterans already managing service-related injuries or PTSD, sleep apnea compounds these challenges. The exhaustion makes physical therapy harder. The brain fog interferes with therapy sessions. The irritability strains family relationships you’re trying to rebuild.

Understanding VA Disability Ratings for Sleep Apnea
The VA rates sleep apnea under diagnostic code 6847 in the Schedule for Rating Disabilities. Your rating determines your monthly compensation and reflects how severely the condition impacts your ability to work and function.
Current rating structure (as of 2026):
100% Rating:
- Requires a tracheostomy (surgical breathing hole in your neck)
- OR chronic respiratory failure with cor pulmonale (right-sided heart failure from lung disease)
- Monthly compensation: $3,737.85 (single veteran with no dependents)
50% Rating:
- Requires use of a breathing assistance device such as CPAP (Continuous Positive Airway Pressure)
- This is the most commonly awarded rating for veterans with sleep apnea
- Monthly compensation: $1,075.16
30% Rating:
- Persistent daytime hypersomnolence (excessive sleepiness)
- Documented through sleep studies and medical records
- Monthly compensation: $524.31
0% Rating:
- Sleep apnea is documented and diagnosed
- Currently asymptomatic or symptoms don’t require treatment
- No monthly compensation, but establishes service connection for future claims
What determines your rating:
The VA looks at your sleep study results (AHI score—apnea-hypopnea index), your symptoms, and most importantly, what treatment you require. If you’re prescribed a CPAP and use it regularly, you’ll typically receive the 50% rating. If you’re prescribed a CPAP but don’t use it consistently, the VA may reduce your rating to 30% or even 0%.
This creates a critical point: compliance with treatment protects your rating. Use your CPAP every night, keep your medical appointments, and maintain documentation of your treatment adherence.
How to Establish Service Connection for Your Sleep Apnea Claim
Service connection means proving your sleep apnea is linked to your military service. This is where most claims fail—not because veterans don’t have sleep apnea, but because they can’t document the connection clearly enough for the VA.
Three paths to service connection:
1. Direct Service Connection
Your sleep apnea began during service or is directly caused by service conditions:
- Burn pit or toxic exposure during deployment
- Head, neck, or jaw injuries that altered your airway
- Development of obesity due to service-connected disabilities
- Documented sleep problems that began during active duty
2. Secondary Service Connection
Your sleep apnea developed as a result of another service-connected condition:
- PTSD causing sleep disturbances that led to sleep apnea
- Service-connected injuries limiting physical activity, causing weight gain
- Medications for service-connected conditions that contributed to sleep apnea
- Rhinitis or sinusitis from deployment exposure
3. Presumptive Service Connection
For certain veterans, the VA presumes service connection without requiring you to prove the link. This currently applies to some conditions related to burn pit exposure, though sleep apnea isn’t automatically presumptive. However, the PACT Act (passed in 2022, expanded through 2026) has made it easier to establish connection for respiratory conditions related to toxic exposure.
Evidence you need:
- Current diagnosis: Sleep study results showing you have sleep apnea, including your AHI score
- In-service event or injury: Service medical records, deployment records, burn pit registry documentation
- Medical nexus: A doctor’s opinion (nexus letter) stating it’s “at least as likely as not” that your sleep apnea is related to your service
- Lay statements: Your own statement and statements from family members describing when symptoms began and how they’ve progressed
Common mistakes that lead to denial:
- Claiming sleep apnea without a formal sleep study diagnosis
- Failing to connect the condition to a specific service event or exposure
- Not obtaining a nexus letter from a qualified medical professional
- Incomplete service medical records
- Waiting too long after separation to file (though there’s no absolute deadline, earlier claims are easier to prove)
The VA Claims Process: Step-by-Step
Filing a successful sleep apnea claim requires organization and patience. Here’s the process broken down:
Step 1: Get diagnosed
Before filing, see your doctor and get a sleep study. The VA can’t rate a condition you haven’t been diagnosed with. Your sleep study should include:
- Polysomnogram (PSG) results
- AHI score (number of apnea/hypopnea events per hour)
- Oxygen saturation levels
- Sleep architecture analysis
- Treatment recommendations
Step 2: Gather service records
Request your complete service medical records and personnel file. Look for:
- Any mentions of sleep problems, snoring, or fatigue during service
- Deployment locations and dates (especially Iraq, Afghanistan, or other burn pit locations)
- Injuries to head, neck, jaw, or nose
- Diagnoses of conditions that could lead to sleep apnea
Step 3: Obtain a nexus letter
This is often the make-or-break document. A qualified physician (MD or DO, preferably a sleep specialist) reviews your service records and current diagnosis, then writes an opinion letter stating whether your sleep apnea is related to service. The key phrase: “It is at least as likely as not (50% or greater probability) that the veteran’s sleep apnea is related to military service.”
Step 4: File your claim
Submit VA Form 21-526EZ (Application for Disability Compensation) through:
- VA.gov (fastest method)
- Mail to your regional VA office
- In person at a VA regional office
- Through a Veterans Service Organization (VSO)
Include all supporting evidence: sleep study, service records, nexus letter, lay statements.
Step 5: Attend C&P exam
The VA will schedule a Compensation & Pension exam with one of their doctors. This doctor will:
- Review your medical history
- Ask about your symptoms
- Examine you physically
- Review your sleep study results
- Write an opinion about your condition and its severity
Be honest and thorough. Describe your worst days, not your best. Explain how sleep apnea affects your work, relationships, and daily activities.
Step 6: Wait for decision
Initial decisions typically take 3-6 months, though complex cases can take longer. The VA will send a decision letter explaining:
- Whether your claim was approved or denied
- Your disability rating if approved
- The effective date (usually your claim filing date)
- Your right to appeal if denied
Step 7: Appeal if necessary
If denied or given a lower rating than expected, you have one year to file a Supplemental Claim (with new evidence) or request a Higher-Level Review. Consider working with a VA-accredited attorney or VSO for appeals—success rates improve significantly with professional help.

Treatment Options That Actually Work
Getting your VA rating is important, but treating your sleep apnea is essential for your health. Multiple effective options exist, and what works best depends on your specific situation.
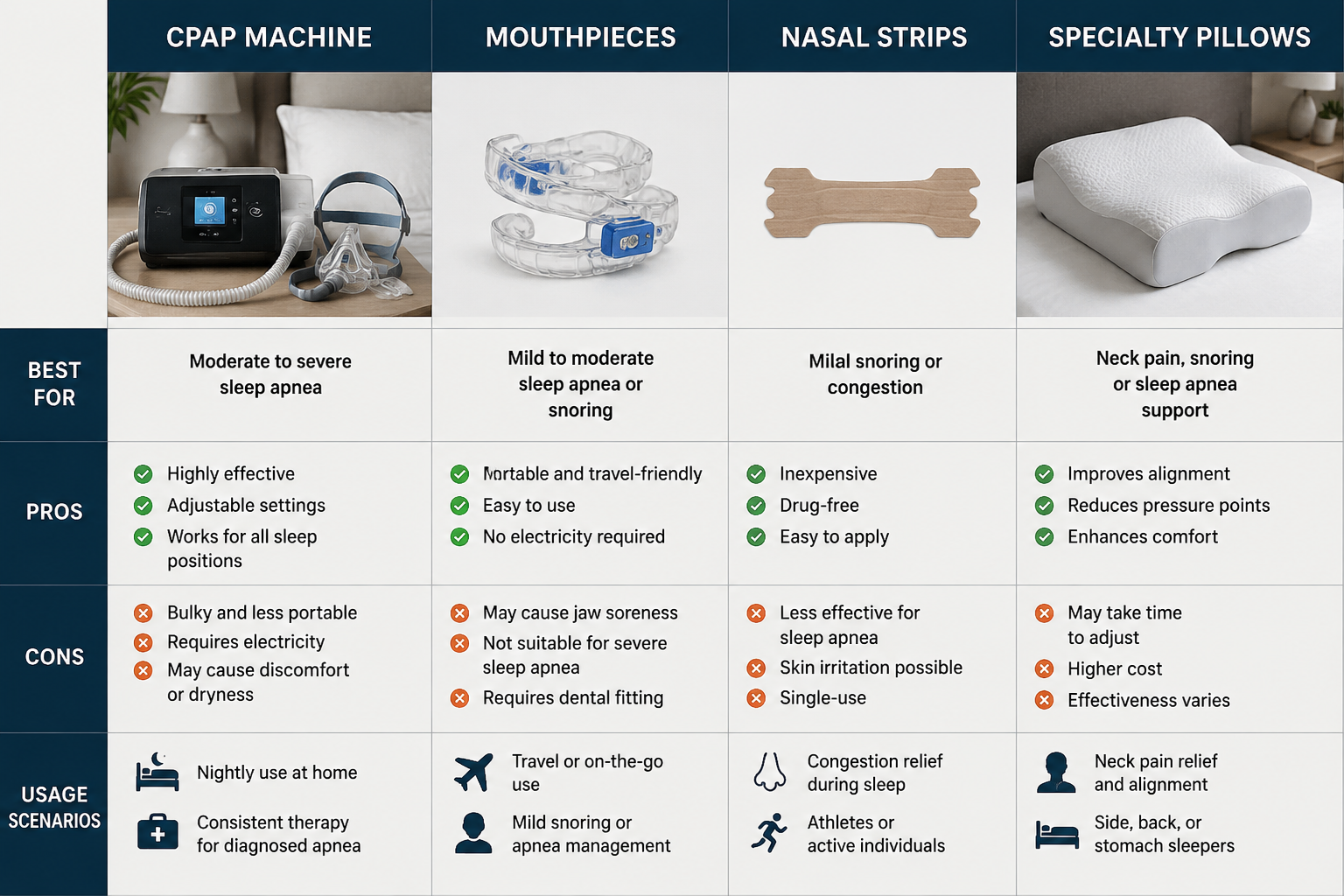
CPAP Therapy: The Gold Standard
Continuous Positive Airway Pressure (CPAP) remains the most effective treatment for moderate to severe obstructive sleep apnea. A CPAP machine delivers steady air pressure through a mask, keeping your airway open throughout the night.
How it works:
The machine sits on your nightstand and connects via tube to a mask covering your nose, mouth, or both. The gentle air pressure acts as a pneumatic splint, preventing your airway from collapsing.
Benefits:
- Immediately eliminates apnea events in most users
- Reduces snoring by 90%+
- Improves daytime alertness within days
- Lowers blood pressure
- Reduces heart attack and stroke risk
- Qualifies you for 50% VA disability rating
Challenges:
- Takes 2-4 weeks to adjust to wearing a mask
- Requires nightly use (every single night)
- Needs regular cleaning and maintenance
- Mask leaks can be frustrating initially
- Some people feel claustrophobic
VA coverage:
The VA provides CPAP machines, masks, supplies, and ongoing support at no cost to veterans with service-connected sleep apnea. You’ll receive replacement supplies regularly and can try different mask styles until you find one that works.
Success tip: Use your CPAP every night, even for naps. The VA tracks compliance through machine data. Consistent use protects your disability rating and, more importantly, your health.
Oral Appliances and Mouthpieces
For mild to moderate sleep apnea, or for people who can’t tolerate CPAP, dental devices offer an effective alternative. These anti-snoring mouthpieces work by repositioning your jaw or tongue to keep your airway open.
Mandibular Advancement Devices (MADs):
These devices push your lower jaw forward, which pulls your tongue away from the back of your throat. Popular options include custom-fitted devices from dentists or over-the-counter options like SnoreRx and VitalSleep.
Tongue Retaining Devices (TRDs):
These hold your tongue forward using gentle suction. The Good Morning Snore Solution is the most researched TRD and works well for people with jaw problems who can’t use MADs.
Pros:
- Portable and travel-friendly
- No electricity required
- Quieter than CPAP
- Lower maintenance
- Effective for mild-moderate OSA
Cons:
- Can cause jaw soreness initially
- May shift teeth with long-term use
- Less effective than CPAP for severe sleep apnea
- Requires proper fitting for effectiveness
VA coverage:
The VA may provide oral appliances through dental services if you qualify for VA dental care and your doctor recommends this treatment.
Positional Therapy and Sleep Position Aids
Many people have positional sleep apnea—their breathing problems occur mainly when sleeping on their back. If your sleep study shows this pattern, positional therapy can help.
Options include:
- Specialty sleep pillows designed to keep you on your side
- Wearable devices that vibrate when you roll onto your back
- Tennis ball technique (sewing a tennis ball into the back of your pajama shirt)
- Adjustable beds that elevate your upper body
Best for:
- Mild sleep apnea that’s worse when supine (on your back)
- Supplementing other treatments
- People who naturally sleep on their side most of the night
Nasal Devices and Breathing Aids
Provent and Theravent:
These small adhesive valves fit over your nostrils. They open when you inhale but create resistance when you exhale, which keeps your airway open. Provent requires a prescription; Theravent is over-the-counter.
Nasal strips:
External strips that lift and open nasal passages. Effective for snoring caused by nasal congestion but less helpful for true sleep apnea. Inexpensive and worth trying as a supplemental treatment.
Nasal dilators:
Internal devices that hold nostrils open from inside. Useful if nasal congestion contributes to your sleep apnea.
Surgical Options
When other treatments fail or specific anatomical problems exist, surgery may help:
Uvulopalatopharyngoplasty (UPPP):
Removes excess tissue from your throat. Success rates vary (40-60%), and recovery takes 2-3 weeks.
Maxillomandibular advancement:
Moves your jaw forward permanently. More invasive but highly effective for severe OSA (80-90% success rate).
Inspire therapy:
An implanted device that stimulates your tongue nerve to keep your airway open. FDA-approved for moderate-severe OSA in people who can’t tolerate CPAP.
Nasal surgery:
Corrects deviated septum or removes polyps that block breathing.
The VA covers medically necessary sleep apnea surgeries for veterans with service-connected conditions.
Lifestyle Changes That Help
While rarely sufficient alone, these changes improve treatment effectiveness:
- Weight loss: Losing 10% of body weight can reduce AHI by 30% or more
- Avoid alcohol: Especially within 3 hours of bedtime (relaxes throat muscles)
- Quit smoking: Smoking increases airway inflammation and fluid retention
- Sleep schedule: Consistent bed and wake times improve sleep quality
- Exercise: 30 minutes daily improves sleep apnea severity
- Treat allergies: Reduces nasal congestion that worsens breathing
Common Symptoms: How to Know If You Have Sleep Apnea
Many veterans live with sleep apnea for years without realizing it. The condition only occurs during sleep, so you might not notice the breathing pauses yourself.
Classic warning signs:
During sleep (often noticed by a partner):
- Loud, chronic snoring that disrupts others
- Gasping or choking sounds
- Breathing pauses lasting 10+ seconds
- Restless sleep with frequent position changes
- Night sweats
Upon waking:
- Dry mouth or sore throat
- Morning headaches
- Feeling unrefreshed despite adequate time in bed
- Difficulty waking up
During the day:
- Overwhelming sleepiness, especially during quiet activities
- Falling asleep while driving, watching TV, or in meetings
- Difficulty concentrating or remembering
- Irritability, mood swings, or depression
- Decreased libido
Physical signs:
- Neck circumference over 17 inches (men) or 16 inches (women)
- High blood pressure resistant to medication
- Obesity, especially around the neck and upper body
- Recessed chin or small jaw
- Large tongue or tonsils
If you recognize three or more of these symptoms, talk to your doctor about a sleep study. Don’t wait—untreated sleep apnea damages your health progressively.
Getting Diagnosed: What to Expect from a Sleep Study
Formal diagnosis requires a sleep study (polysomnography). Your primary care doctor can refer you to a sleep specialist who will order the appropriate test.
Two types of sleep studies:
In-lab polysomnogram (PSG):
You spend the night at a sleep center while technicians monitor you. Sensors track:
- Brain waves (EEG)
- Eye movements
- Heart rate and rhythm
- Blood oxygen levels
- Breathing rate and effort
- Muscle activity
- Body position
- Snoring sounds
This comprehensive test is the gold standard and required for complex cases or when other sleep disorders are suspected.
Home sleep apnea test (HSAT):
You take portable equipment home and sleep in your own bed. The device monitors breathing, oxygen levels, heart rate, and sometimes body position. Less comprehensive than in-lab testing but adequate for diagnosing straightforward obstructive sleep apnea.
What your results mean:
Your AHI (Apnea-Hypopnea Index) score indicates severity:
- Normal: AHI less than 5 events per hour
- Mild: AHI 5-14 events per hour
- Moderate: AHI 15-29 events per hour
- Severe: AHI 30+ events per hour
The VA considers both your AHI score and your symptoms when assigning a disability rating. Someone with an AHI of 20 who uses CPAP receives the same 50% rating as someone with an AHI of 60 who uses CPAP.
For VA claims purposes:
Make sure you receive a complete copy of your sleep study report. This document is essential evidence for your disability claim. If possible, have your sleep study done through the VA healthcare system—this creates an automatic record in your VA medical file.
Why Three Out of Four Claims Get Denied (And How to Avoid It)
The VA denies approximately 75% of initial sleep apnea claims. Understanding why helps you build a stronger case from the start.
Top reasons for denial:
1. Insufficient medical evidence
Filing without a formal sleep study diagnosis or with incomplete documentation. The VA needs objective evidence—your word alone isn’t enough.
Fix: Get a complete sleep study before filing. Ensure your medical records clearly document your diagnosis, AHI score, and treatment plan.
2. Missing service connection
You have sleep apnea, but you haven’t proven it’s related to military service. This is the most common denial reason.
Fix: Obtain a strong nexus letter from a qualified physician. Document your service conditions (burn pit exposure, deployment stress, service injuries). Provide lay statements describing when symptoms began.
3. Lack of current symptoms
The VA determines you have sleep apnea but it’s not currently causing problems or requiring treatment.
Fix: Be thorough during your C&P exam. Describe your worst symptoms, not your best days. Explain how the condition affects your work, relationships, and daily activities. If you’re using CPAP, emphasize that you require it to function normally.
4. Incomplete service medical records
Your service records don’t show any sleep-related complaints or relevant injuries/exposures.
Fix: File a claim anyway if you believe service caused your condition. Use lay statements to fill gaps. Consider a private medical opinion if service records are incomplete.
5. Failure to attend C&P exam
Missing your scheduled exam without rescheduling results in automatic denial.
Fix: Attend all scheduled exams. If you must reschedule, contact the VA immediately. Treat the C&P exam as seriously as a job interview—your benefits depend on it.
Working with professionals:
Veterans Service Organizations (VSOs) like DAV, VFW, and American Legion provide free help with claims. They know the system, understand what evidence the VA needs, and can guide you through the process.
For denied claims or complex cases, consider hiring a VA-accredited attorney. They work on contingency (paid from back pay only if you win) and significantly improve success rates on appeals.
Frequently Asked Questions
Can I get VA disability for sleep apnea if I didn’t have symptoms during service?
Yes. Many conditions, including sleep apnea, develop months or years after service ends. You need to establish that service conditions caused or contributed to the condition, even if symptoms appeared later. Burn pit exposure, for example, can cause respiratory damage that leads to sleep apnea years after deployment.
What if I’m already receiving CPAP from the VA but don’t have a disability rating?
File a claim immediately. Receiving treatment through VA healthcare doesn’t automatically grant you disability compensation—you must file a separate claim. Your existing VA medical records showing diagnosis and treatment will support your claim.
Does obesity disqualify me from service connection?
No. While obesity can cause sleep apnea, the VA recognizes that service conditions often contribute to weight gain (injuries limiting activity, medications, stress). If you can show your obesity resulted from service-connected conditions, or that you had sleep apnea risk factors during service, you can still establish service connection.
How long does a sleep apnea claim take?
Initial claims typically take 3-6 months, though this varies by region and claim complexity. Appeals can take 1-3 years depending on the appeal type. Filing online through VA.gov tends to be faster than paper applications.
Can my rating increase over time?
Yes. If your sleep apnea worsens or you develop complications, you can file for an increased rating. For example, if you initially received 30% for daytime sleepiness but now require CPAP, you can request an increase to 50%. File a new claim with updated medical evidence showing the increased severity.
What if I can’t tolerate CPAP—will I lose my 50% rating?
Not necessarily. If you genuinely cannot tolerate CPAP despite trying multiple masks and settings, document this thoroughly with your doctor. You may maintain your 50% rating if medical records show you require CPAP but cannot use it due to medical reasons. However, if you simply choose not to use it without medical justification, the VA may reduce your rating.
Can I get sleep apnea rated as secondary to PTSD?
Yes. PTSD commonly causes sleep disturbances that can lead to or worsen sleep apnea. You’ll need medical evidence (a nexus letter) establishing the connection between your service-connected PTSD and your sleep apnea. Many veterans successfully claim sleep apnea secondary to PTSD.
Do I need to use my CPAP every single night?
For optimal health, yes. For maintaining your VA rating, the VA may review compliance data from your CPAP machine. Most sleep doctors recommend using CPAP at least 4 hours per night, at least 70% of nights. However, for your health benefits, aim for every night, all night.
What’s the monthly compensation for a 50% sleep apnea rating?
As of 2026, a single veteran with no dependents receives $1,075.16 monthly for a 50% rating. Veterans with dependents receive more. Rates increase annually based on cost-of-living adjustments.
Can I work while receiving sleep apnea disability?
Yes. VA disability compensation is not based on your ability to work—it’s compensation for service-connected conditions. You can work full-time and still receive disability benefits. The rating reflects the severity of your condition and required treatment, not your employment status.
Should I file for sleep apnea even if I’m not sure it’s service-connected?
Yes. File the claim and let the VA evaluate the evidence. The worst outcome is denial, which you can appeal. Many veterans are surprised to learn their condition qualifies for service connection. Don’t self-reject—file and provide the best evidence you can gather.
How do I prove burn pit exposure?
Register in the Airborne Hazards and Open Burn Pit Registry (if you haven’t already). Provide deployment records showing you served in locations with burn pits (Iraq, Afghanistan, and other Middle East locations from 1990-present). The PACT Act has made it easier to establish presumptive service connection for respiratory conditions related to burn pit exposure.
Final Thoughts: You’ve Earned These Benefits
If you served your country and now struggle with sleep apnea, you deserve both effective treatment and fair compensation. The VA disability system can be frustrating and complex, but don’t let that discourage you from filing a claim.
Remember these key points:
- Get formally diagnosed with a sleep study before filing
- Document the connection between your service and your condition
- Obtain a strong nexus letter from a qualified physician
- Be thorough and honest during your C&P exam
- Don’t give up if initially denied—appeal with additional evidence
- Use your treatment consistently, both for your health and your rating
- Consider working with a VSO or attorney for complex claims
Your sleep apnea isn’t just an inconvenience—it’s a serious medical condition that affects every aspect of your life. Proper treatment can dramatically improve your energy, mood, relationships, and long-term health. The VA benefits you’re entitled to can help support you while you manage this condition.
Whether you’re just beginning to suspect you have sleep apnea or you’ve been denied a claim and need to appeal, take action today. Talk to your doctor, gather your evidence, and file your claim. You’ve served your country—now let your country serve you.